Abstract
Background
To date, there are insufficient data on long-term outcomes of weight loss surgery in children and adolescents with obesity beyond 5 years of follow-up. This study aimed to analyze durability of weight loss and comorbidity resolution, growth velocity, and adverse events associated with laparoscopic sleeve gastrectomy (LSG) in children and adolescents with severe obesity.
Study Design
In this prospective cohort study, 2,504 children and adolescents with class II/III obesity who were enrolled in a multidisciplinary, family-based pediatric obesity management program underwent LSG between 2008 and 2021. Weight loss, growth, comorbidity resolution, and adverse event data during the first 10 years after LSG were analyzed.
Results
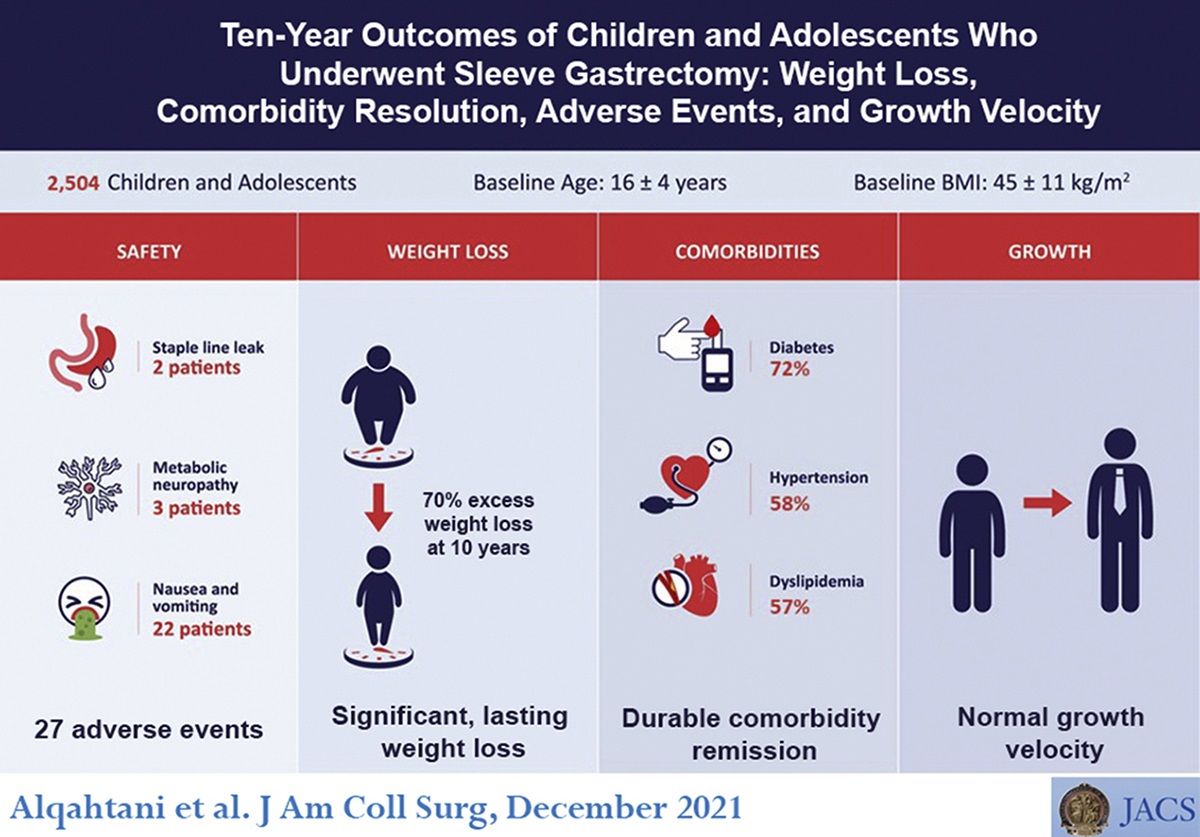
The cohort age was 5 to 21 years at the time of operation, and 55% were female. Mean ± SD percentage of excess weight lost during short- (1 to 3 years; n = 2,051), medium- (4 to 6 years; n = 1,268), and long-term (7 to 10 years; n = 632) follow-up was 82.3% ± 20.5%, 76.3% ± 29.1%, and 71.1% ± 26.9%, respectively. Complete comorbidity remission at long-term follow-up was observed in 74%, 59%, and 64% of type 2 diabetes, dyslipidemia, and hypertension cases, respectively. Mean ± SD height z-score change at short-, medium-, and long-term follow-up was 0.1 ± 0.5, 0.1 ± 1.2, and 0.0 ± 0.8, respectively, representing no significant change in growth velocity. There were 27 adverse events (1%) with no procedure-related mortality.
Conclusions
Long-term follow-up after LSG in children and adolescents demonstrates durable weight loss, maintained comorbidity resolution, and unaltered growth.
References:
The study was published in (JACS. JOURNAL OF THE AMERICAN COLLEGE OF SURGEONS)